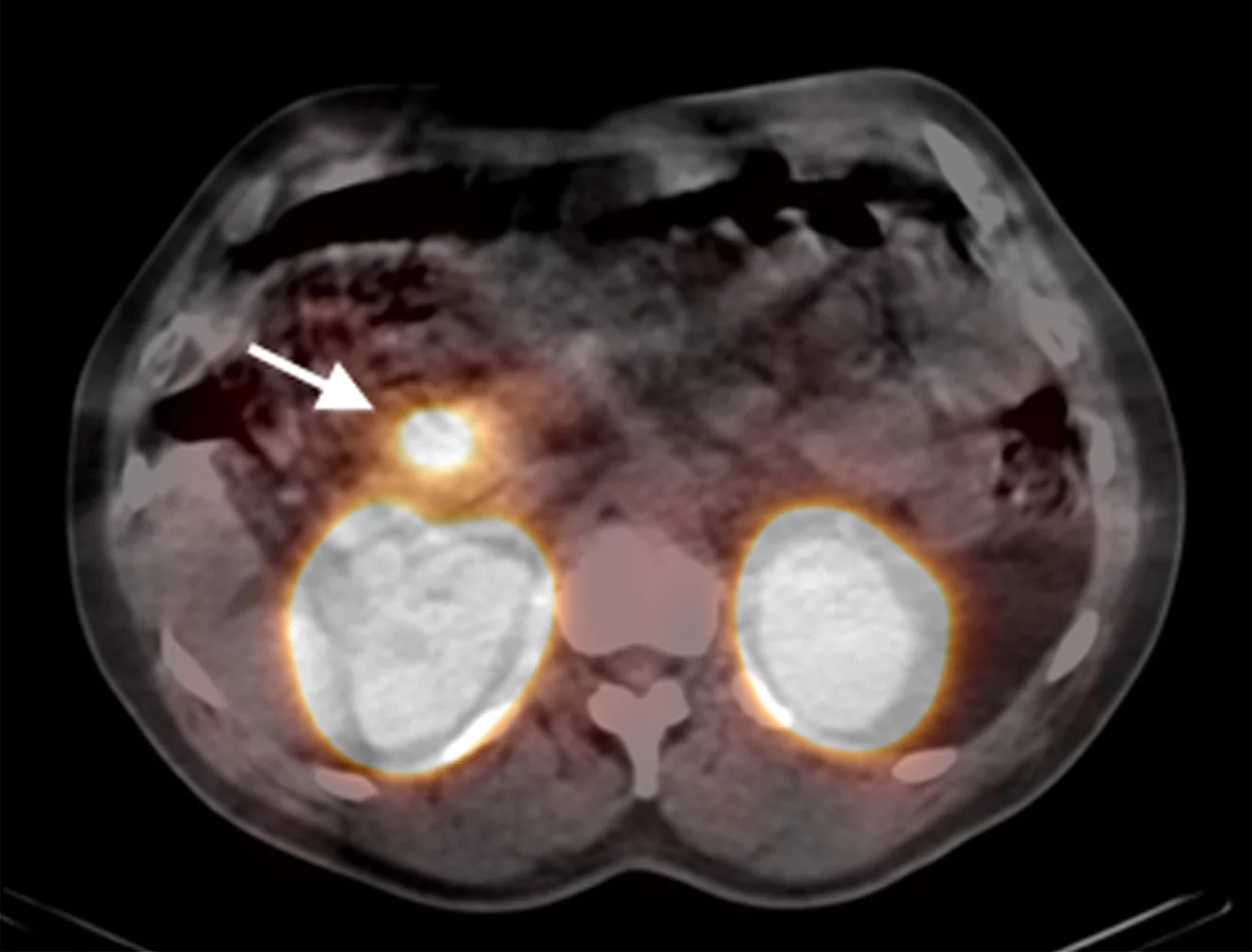
Besser als CT und MRT: Forschende des Inselspitals Bern, des Universitätsspitals Basel und des Paul Scherrer Instituts haben eine neue Methode zur Erkennung kleiner Tumore in der Bauchspeicheldrüse entwickelt.
Schweizer Forschende haben eine Methode entwickelt, die bestimmte Tumore in der Bauchspeicheldrüse, sogenannte Insulinome, zuverlässig lokalisieren kann. Deren Erfolg wird im September in der Diabetes-Ausgabe der renommierten Medizinzeitschrift Lancet publiziert. Die Studie wurde vom Schweizerischen Nationalfonds, der Krebsliga Schweiz und dem United Kingdom Department of Health unterstützt.
Gefährliche Unterzuckerungen
Insulinome sind seltene Tumore, die Hormone, insbesondere Insulin, produzieren. Sie befinden sich normalerweise in der Bauchspeicheldrüse (Pankreas) und sind meistens gutartig und klein (ca. 1 bis 1.5 cm im Durchmesser). Da sie aber unreguliert Insulin ausschütten, verursachen sie immer wieder gefährliche Unterzuckerungen (Hypoglykämien), die zu Verwirrtheit, Krampfanfällen und Bewusstseinsverlust bis zum Koma führen können. Oft dauert es lange, bis die Diagnose gestellt wird. Für die Patienten bedeutet dies eine lange und intensive Leidenszeit.
Operieren – aber wo?
Die einzige Heilung ist die operative Entfernung des Insulinoms. Dazu braucht der Chirurg die genaue Lokalisation des Tumors. Mit der konventionellen Bildgebung via CT (Computer-Tomographie) und MRT (Magnetresonanz-Tomographie) können 60 bis 70 Prozent dieser Tumore lokalisiert werden. 30 bis 40 Prozent bleiben unentdeckt. Weiterführende Abklärungen waren bisher sehr aufwändig: Zur Messung des Insulins muss ein Katheter in die Pankreas-Gefässe oder die Leber-Vene eingeführt werden, und zur Feststellung eines kleinen Tumors braucht es eine Magenspiegelung mit Ultraschall in der Bauchspeicheldrüse.
Tumor radioaktiv sichtbar gemacht
Um den Insulinomen auf die Schliche zu kommen, haben die Forscher 30 Patienten mit dringendem Insulinom-Verdacht eine künstliche Substanz injiziert, verbunden mit schwach radioaktivem Indium. Die Substanz wird vom Tumor aufgenommen, und dank der schwachen radioaktiven Strahlung ist die Mini-Geschwulst in einer Spezial-Kamera gut sichtbar. So konnten 95 Prozent der Insulinome lokalisiert werden. Mit CT oder MRT waren es lediglich 47 Prozent. Klinischer Forschungsleiter Prof. Emanuel Christ vom Inselspital Bern: „Es ist wahrscheinlich, dass diese Methode in Zukunft die bisherigen Methoden der Lokalisation von Insulinomen ablösen wird.“
Erfolg dank internationalem Netzwerk
Was sich so einfach anhört, war nur dank jahrelanger Vorarbeit und einem internationalen Forschungs-Netzwerk möglich: Am Inselspital und am Universitätsspital Basel definierten der Diabetologe Prof. Emanuel Christ und die Nuklearmediziner Prof. Damian Wild und PD Dr. Flavio Forrer das Ziel der Studie, die Studienmethode und die Kriterien für die Patientenauswahl, danach wählten sie und Kollegen in St. Gallen, Luzern, Freiburg im Breisgau (D) und London Patienten für die Studie aus. 2009 bestätigten die Forschenden ihre Hypothese erstmals mit sechs Patienten. Die grosse Studie diente danach der Vertiefung.
Tumor überlistet mit Schlüsselloch-Technik
Dr. Martin Behé (jetzt am Paul-Scherrer-Institut) und Kollegen entwickelten eine radioaktive Substanz, um den unsichtbaren Tumor zu überlisten. Sie machten sich dabei ein bekanntes Phänomen zunutze: Insulinome haben an der Oberfläche sehr viele sogenannte GLP-1-Rezeptoren – eine Art Schlüsselloch, das nur mit einem einzigen Schlüssel, der chemischen Substanz GLP-1, geöffnet werden kann. Die Forscher verwendeten eine von ihnen mitentwickelte ähnliche Substanz, Exendin-4, die ins gleiche „Schlüsselloch“ passt. Mit dem Exendin-4 konnte das schwach radioaktive Indium in den Tumor geschmuggelt und dessen Tarnkappe gelüftet werden.
Text: Inselspital Bern, Universitätsspital Basel, PSI
Über das PSI
Das Paul Scherrer Institut entwickelt, baut und betreibt grosse und komplexe Forschungsanlagen und stellt sie der nationalen und internationalen Forschungsgemeinde zur Verfügung. Eigene Forschungsschwerpunkte sind Materie und Material, Mensch und Gesundheit, sowie Energie und Umwelt. Mit 1500 Mitarbeitenden und einem Jahresbudget von rund 300 Mio. CHF ist es das grösste Forschungsinstitut der Schweiz.
Kontakt / Ansprechpartner
Prof. Dr. Emanuel Christ, Inselspital, Universitätsspital Bern, Universitätspoliklinik für Endokrinologie, Diabetologie und Klinische Ernährung,E-Mail: Emanuel.Christ@insel.ch
Prof. Dr. Damian Wild, Universitätsspital Basel, Abteilung für Nuklearmedizin / Universitätsklinikum Freiburg / University College London Hospital,
E-Mail: Damian.Wild@usb.ch
Dr. Martin Béhé, Paul Scherrer Institut, Zentrum für radiopharmazeutische Wissenschaft / Universitätsklinikum Freiburg,
Telefon: 056 310 28 17, E-Mail: martin.behe@psi.ch
Originalveröffentlichung
Glucagon-like peptide-1 receptor imaging for the localisation of insulinomas: a prospective multicentre imaging studyProf Emanuel Christ, Prof Damian Wild, Susanne Ederer, Martin Béhé PhD, Guillaume Nicolas, Prof Martyn E Caplin, Prof Michael Brändle, Thomas Clerici, Stefan Fischli, Prof Christoph Stettler, Prof Peter J Ell, Prof Jochen Seufert, Prof Beat Gloor, Prof Aurel Perren, Prof Jean Claude Reubi, Flavio Forrer
The Lancet Diabetes & Endocrinology, Early Online Publication, 25 July 2013
http://www.thelancet.com/journals/landia/onlinefirst