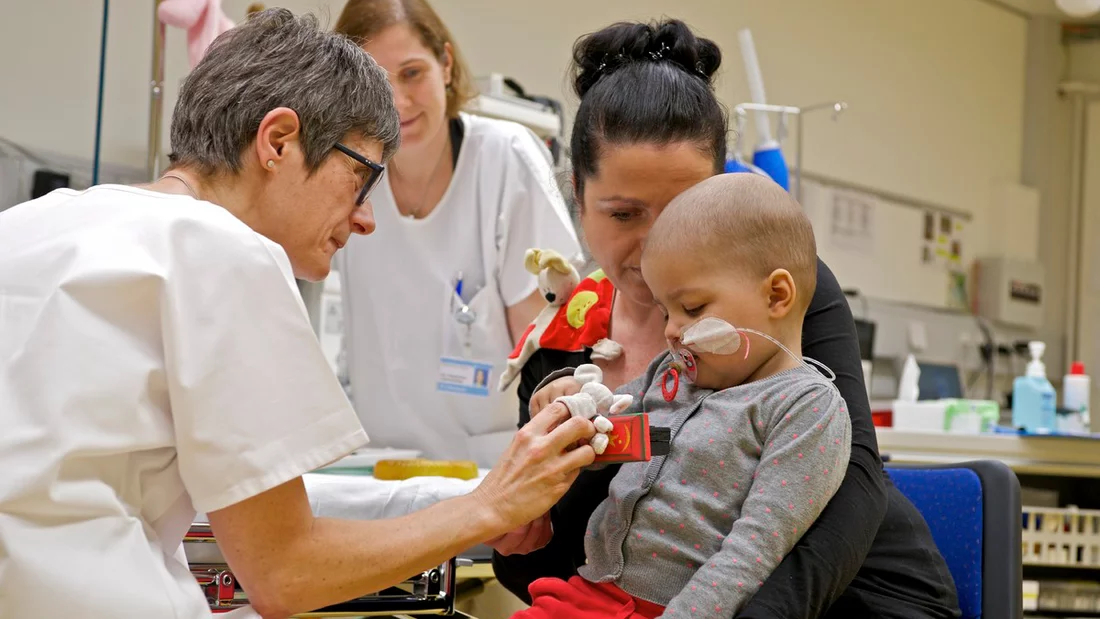
Krebs bei Kindern ist selten. Dennoch treten insbesondere bösartige Tumore von Muskeln, Knochen und Nervengewebe schon bei den Kleinsten auf. Dann ist jede Behandlung eine Gratwanderung. Weil das Kind noch wächst und die sich entwickelnden Organe Schaden nehmen können, sind herkömmliche Bestrahlungen und die meisten Chemotherapien mit grossen Nebenwirkungen verbunden. Die Ärzte am Zentrum für Protonentherapie am Paul Scherrer Institut PSI behandeln krebskranke Kinder daher mit Protonenstrahlen. Protonen erlauben eine sanftere Bestrahlung des Krebses und treffen den Tumor millimetergenau; gesundes Gewebe hingegen wird geschont. Bis heute hat das PSI damit schon über 450 Kinder behandelt.
Irgendetwas stimmte nicht. Dieses seltsame Druckgefühl hinter dem Auge war neu. Das Sehen ging schlechter, und manchmal tat der Kopf weh. Der achtjährige Junge war unsicher. Ob er sich alles nur einbildete? Doch auch drei Wochen später wurde es nicht besser, sodass er schliesslich gemeinsam mit seinen Eltern zum Arzt ging. Viele Untersuchungen später stand die vernichtende Diagnose fest: Rhabdomyosarkom. Unter diesem Fachbegriff fassen Ärzte bösartige Tumore zusammen, die von weichen Gewebestrukturen wie Muskeln oder Bindegewebe ausgehen. Sie kommen hauptsächlich bei Kindern vor und wuchern am häufigsten im Kopf- und Halsbereich, aber auch am Becken und an anderen Stellen des Körpers. Grundsätzlich lassen sie sich genauso behandeln wie Krebs bei Erwachsenen: mit einer Operation, Chemotherapie, Bestrahlung oder Kombinationen davon. Trotzdem gibt es Grenzen. Wenn etwa ein Auge oder der Hirnstamm in unmittelbarer Nähe liegen, wollen die Betroffenen oftmals keine Operation, da sie zu Blindheit, Lähmungen oder anderen schweren Beeinträchtigungen führen könnte. Und eine herkömmliche Strahlentherapie würde zu viele gesunde Zellen in der Nähe des Tumors schädigen. Nicht so die Protonenbestrahlung mit der Spot-Scanning-Technik.
Bei diesem Verfahren, das Forschende vor zwanzig Jahren am Paul Scherrer Institut PSI entwickelt haben, wird das ganze Volumen eines Tumors von einem Strahl aus Protonen millimetergenau abgerastert. Die Protonen können so zielgerichtet platziert werden, dass sie ihre maximale Wirkung nur in den Krebszellen entfalten. Gesundes Gewebe, welches den Tumor umgibt, wird dadurch geschont. Eines der ersten Kinder, das wir hier behandelt haben, war ein fast 2-jähriger Junge, der ein Rhabdomyosarkom in der Augenhöhle hatte. Dieser Tumor lag sehr ungünstig. So stand er vor der Wahl, sich einer sehr entstellenden Operation am Gesicht unterziehen zu müssen oder zu einer Protonentherapie zu uns zu kommen
, sagt Lydia Lederer, medizinisch-technische Radiologieassistentin am Zentrum für Protonentherapie ZPT des PSI. Die Behandlung hat dem Kind damals das Leben gerettet, und auch das Gesicht wurde nicht entstellt.
Das war vor 13 Jahren. Seitdem wurden am ZPT rund 450 Kinder mit Protonen behandelt. Viele von ihnen hatten einen Tumor im Kopf oder an der Wirbelsäule, also genau an solchen Körperstellen, deren benachbarte Gewebe oder Organe möglichst keiner Strahlung ausgesetzt werden dürfen. Lederer, die seit 15 Jahren dabei ist, hat mehrere Hundert dieser Kinder bei ihrer Strahlentherapie begleitet. Das jüngste war gerade einmal neun Monate alt.
Patienten vom anderen Ende der Welt
Wenn Kinder so klein sind und Krebs haben, kommt das einem Ausnahmezustand für die ganze Familie gleich. Viele Eltern haben nicht nur Angst um ihr Kind, sondern fühlen sich mit der Situation überfordert. Die Behandlung dauert mehrere Wochen, und sie sind häufig weit weg von Zuhause. Deshalb versucht das Team am ZPT, die Kinder samt Familien bestmöglich zu unterstützen. Manchmal ist das gar nicht so einfach, denn viele Kinder kommen extra aus dem Ausland und sprechen kein Deutsch. Das ZPT hat weltweit einen so hervorragenden Ruf, dass sogar Ärzte aus weit entfernten Ländern wie Australien ihre kleinen Patienten nach Villigen überweisen. Wir haben uns mittlerweile sehr gut auf die ausländischen Patienten eingestellt und finden am PSI immer jemanden, der die Muttersprache des Kindes kann
, sagt Lederer, die extra für ihre Patienten Italienisch gelernt hat.
Modernste Therapie und warmherzige Fürsorge
Mehrsprachigkeit ist für die Mitarbeitenden am ZPT selbstverständlich. Ebenso wichtig ist jedoch, dass sie ihren Patienten helfen, den ganzen Aufenthalt zu organisieren. Zudem machen sie Abklärungen mit den Krankenkassen sowie den Ärzten und unterstützen die Familie bei den Behörden. Am wichtigsten ist jedoch, dass sie den Kindern helfen können und diese sich trotz Krebsdiagnose wohlfühlen. Viele kleine, liebevolle Details am ZPT zaubern bei den kleinen Patienten ein Lächeln hervor. So hängt im Wartezimmer eine Sonne an der Wand, an der Tür klebt ein Giraffenbild, und über die Fenster klettern gemalte Affen. Regale voller Comics und Kinderbücher, Spielzeug und Murmelbahnen lenken die Kleinen vom eigentlichen Zweck ihres Aufenthaltes ab. Denn im Grunde passt es nicht zusammen – Krebsbehandlung und ein neugieriges, quirliges Kind. Kinder wollen vor allem spielen und fröhlich sein. Für mich als Arzt ist es besonders wichtig, dass ich dem Kind versprechen kann, dass ich ihm nicht weh tue
, betont Fritz Murray, der sich am ZPT zum Radioonkologen weiterbildet. Die Strahlentherapie ist unsichtbar und man spürt sie nicht. Die Kinder fühlen sich bei uns wohl, obwohl wir eine hochtechnische Einrichtung sind.
Entscheidend für den Erfolg des ZPT sei laut Murray, dass es neben der Therapie besonders stark auf Forschung ausgerichtet ist sowie auf höchste Sicherheitsvorkehrungen und Qualität. Gerade diese Punkte sind es, die auch den krebskranken Patienten am meisten zugutekommen.
Gesammeltes Expertenwissen zum Wohle der Kinder
Viele Kinder werden nach genau definierten Bestrahlungsprotokollen behandelt und nehmen an internationalen Studien teil. Dadurch wird einerseits gewährleistet, dass immer das neueste Wissen in die Behandlung einfliesst und dass andererseits nichts dem Zufall überlassen wird. Ob und welches Protokoll bei einem Kind zum Einsatz kommt, hängt von der Art des Tumors und seiner Lage sowie von Faktoren wie etwa dem Alter des Kindes ab. Da einige Tumore extrem selten sind, setzen die Ärzte am ZPT auf das gesammelte Wissen vieler Spezialisten und diskutieren jeden Fall zunächst per Videokonferenz in einem wöchentlichen Gremium mit Kollegen anderer spezialisierter Einrichtungen. Dann wird festgelegt, wie viele Wochen, mit welcher Dosis und an welchen Regionen des Körpers bestrahlt werden muss. Wichtig auch: Gibt es Bereiche in der Nähe des Tumors, die man besonders schonen muss? Ist das Kind alt und reif genug, um jede einzelne Bestrahlung, die manchmal sogar eine Stunde lang dauert, ruhig daliegend und bei vollem Bewusstsein durchzuhalten? Oder ist es vielleicht noch zu klein und braucht eine Narkose? Kinder unter sechs Jahren bekommen meistens eine leichte Narkose zum Schlafen
, erklärt Murray, denn gerade für die Kleinsten ist die Prozedur sonst oftmals zu anstrengend. Deshalb ist immer ein Team von Narkoseärzten des Kinderspitals Zürich mit dabei.
Bei älteren Kindern hingegen ist das nicht nötig: Sie schaffen die Behandlung fast immer ohne Narkose.
Entscheidend für den Erfolg einer Protonentherapie ist die exakte Bestrahlung des Tumors. Dafür muss ein Patient immer in derselben Position liegen und stillhalten. Eine schwierige Aufgabe, besonders für Kinder mit Tumoren im Schädel- oder Halsbereich. Deshalb gibt es zwei Möglichkeiten, sie bei jeder Therapie korrekt unter das Bestrahlungsgerät zu legen: Die eine ist ein sogenannter Beissblock – ein Plastikabdruck vom Gebiss ähnlich wie bei einer Zahnspange. Dieser Abdruck passt dann genau auf die Zähne des Kindes und wird mit einem Gestänge an der Behandlungsliege verbunden. Für die Bestrahlung muss das Kind den Beissblock nur zwischen die Zähne nehmen, wo er mittels Vakuum am Gaumen festgesaugt wird. Somit muss es nicht die ganze Zeit mit eigener Kraft auf den Block beissen, um ihn festzuhalten. Die andere Möglichkeit ist eine an das Gesicht angepasste Maske, mit der das Kind an der Behandlungsliege fixiert wird. Die Kinder kommen mit beiden Varianten recht gut klar
, erklärt Lydia Lederer, die in der Vorbereitung sowohl die Beissblöcke als auch die Masken für die Kinder anformt. Sogar den Teddy oder ein anderes Lieblingskuscheltier des Kindes versorgt sie mit. Der Teddy hat dann wie das Kind eine Maske auf und sitzt während der Bestrahlung neben ihm
, erzählt die Radiologieassistentin, das hilft sehr.
Zusätzlich bekommt jedes Kind ein Quietschtier, mit dem es sich bemerkbar machen kann, wenn es unter dem Bestrahlungsgerät Angst hat oder sich nicht gut fühlt.
Behandlungsgeschichte aus Perlen
Immer wenn eine Bestrahlung vorbei ist, erhält jedes Kind eine kleine Belohnung. Am ZPT gibt es dafür bunte handgefertigte Glasperlen, die am Ende eine wunderschöne Kette ergeben. Dieses Belohnungssystem wird vom Kinderspital Zürich zur Verfügung gestellt. Zu Beginn der Behandlung besteht jede Perlenkette nur aus mehreren würfelförmigen Perlen mit den Buchstaben für den Namen des Kindes. Aber nach jeder Untersuchung und jeder Aufgabe, die der kleine Patient bewältigt hat, gibt es eine neue bunte Perle: für eine Computertomografie zum Beispiel oder wenn die Bestrahlungsmaske angefertigt wurde. Auch nach jeder Bestrahlung kommt eine neue Glasperle hinzu, sodass ganz am Ende, wenn alles vorbei ist, jedes Kind eine eigene Perlenkette hat, die seine ganz persönliche Behandlungsgeschichte erzählt. Es ist eine Geschichte von Angst, Mut, Hoffnung und manchmal Verzweiflung. Denn trotz dieser hochmodernen und sehr wirksamen Protonentherapie überleben nicht alle Kinder. Manchmal ist der Tumor besonders bösartig oder hat schon Tochtergeschwülste gebildet. Lydia Lederer musste lernen, damit umzugehen: Es bedrückt uns sehr, wenn wir erfahren, dass ein Kind den Kampf gegen Krebs verloren hat. Aber trotzdem überwiegen für mich die über sechzig Prozent Kinder, die überlebt haben. Da sage ich mir: Wenn es uns nicht gäbe, würden die vielleicht auch sterben. Das ist der Lichtblick für mich.
Wie glücklich und dankbar viele Kinder und ihre Familien sind, zeigen die zahlreichen bunten Einträge im Gästebuch des ZPT. In vielen Sprachen stehen dort Dankesworte, verziert mit kindlichen Malereien, Aufklebern und Fotos. Diese Einträge und das Wissen, den Kindern geholfen zu haben, sind das Schönste für das Team am ZPT.
Text: Sabine Goldhahn
Weiterführende Informationen
- Einen Überblick über die Arbeit des Zentrums für Protonentherapie (ZPT) und die Entwicklung der Protonentherapie am PSI gibt der Artikel Mehrwert für Krebskranke.
- Eine besondere Form der Protonentherapie, die Spot-Scanning-Technik, wurde vor über zwanzig Jahren am PSI entwickelt. Diese Methode kommt heute weltweit zum Einsatz und hat schon mehreren Tausend Patienten geholfen. Details stehen im Artikel 20 Jahre hochpräzise Krebsbekämpfung.
- Protonentherapie am PSI hat mit der Bestrahlung von Augentumoren begonnen. Bis heute hat das PSI allein 6700 Patienten behandelt. Mehr darüber berichtet der Artikel Lichtblicke für Patienten.
- Für die Sicherheit und hohe Qualität der Protonentherapie am PSI sorgt ein ganzes Team an Spezialisten: Die Sicherheit im Griff.
Kontakt/Ansprechpartner
Dr. Marc Walser, Oberarzt am Zentrum für ProtonentherapiePaul Scherrer Institut, 5232 Villigen PSI, Schweiz
Telefon: +41 56 310 35 24, E-Mail: marc.walser@psi.ch
Lydia Lederer, Leitende MTRA am Zentrum für Protonentherapie
Paul Scherrer Institut, 5232 Villigen PSI, Schweiz
Telefon: +41 56 310 36 53, E-Mail: lydia.lederer@psi.ch
Dr. Ulrike Kliebsch, Verantwortliche für Wissenschaft und Information am Zentrum für Protonentherapie
Paul Scherrer Institut, 5232 Villigen PSI, Schweiz
Telefon: +41 56 310 55 82, E-Mail: ulrike.kliebsch@psi.ch